Volume 6, Issue 2 (2025)
J Clinic Care Skill 2025, 6(2): 71-82 |
Back to browse issues page
Article Type:
Subject:
History
Received: 2025/05/4 | Accepted: 2025/06/10 | Published: 2025/06/18
Received: 2025/05/4 | Accepted: 2025/06/10 | Published: 2025/06/18
How to cite this article
Goudarzi F, Hekmatzadeh F. Systematic Review of Clinical Trials of Herbal Products on Menstrual Bleeding Severity. J Clinic Care Skill 2025; 6 (2) :71-82
URL: http://jccs.yums.ac.ir/article-1-401-en.html
URL: http://jccs.yums.ac.ir/article-1-401-en.html
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



Rights and permissions
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
1- Medicinal Plant Research Center, Yasuj University of Medical Sciences, Yasuj, Iran
Full-Text (HTML) (4158 Views)
Introduction
Heavy menstrual bleeding is a common problem in women that negatively impacts their lifestyle. It is known by terms such as menorrhagia, hypermenorrhea, abnormal uterine bleeding, bleeding due to abnormal uterine function, and excessive uterine bleeding. It is defined as blood loss of more than 80 ml per cycle or a bleeding duration of more than seven days [1]. Between 5% and 29% of women’s visits to the hospital are for heavy menstrual bleeding. Excessive bleeding can interfere with work, daily activities, and social participation. It may also lead to iron deficiency anemia in women. Studies have reported that 18 million young women in the United States have iron deficiency anemia due to heavy bleeding [2]. Anemia can cause complications such as weakness, fatigue, unexplained weight loss, mood swings, and cognitive impairment [3].
Laboratory tests have identified two primary factors in heavy bleeding as excessive fibrinolysis and imbalanced prostaglandin levels [2]. The causes of menorrhagia include hormonal, mechanical, and coagulation disorders, and risk factors include age, racial and cultural groups, number of deliveries, and lifestyle [4]. Many treatments have been proposed for heavy menstrual bleeding, including birth control pills, oral progestins, tranexamic acid, and nonsteroidal anti-inflammatory drugs. Although these drugs may be effective, they have side effects [2].
Surgical procedures include fibroid removal, myomectomy, uterine artery embolization, endometrial ablation, and hysterectomy. These procedures have complications, including repeated treatments, potential serious complications, patient discomfort, and cost; thus, it is essential to have appropriate treatment methods that have minimal side effects and are acceptable to the patient [4]. Therefore, the tendency to use medicinal plants for the treatment of diseases has increased in recent decades [2].
Women have a particular inclination to use herbal medicines for treating diseases and frequently use these remedies to address problems, such as dysmenorrhea, relief of menopausal symptoms, menstrual disorders, mood disorders, prevention of osteoporosis, and issues during pregnancy [5]. Herbal remedies, such as ginger (Zingiber officinale) [2, 5], yarrow (Achillea millefolium) [4], fennel (Foeniculum vulgare) [6], flaxseed (Linum usitatissimum) [3], cumin (Cuminum cyminum) [7], Teucrium polium [8], nettle (Urtica dioica) [9], black seed (Nigella sativa) [10], Golnar (Punica granatum) [11], Cydonia oblonga [12], and chamomile (Matricaria chamomilla) [13] have been used in the treatment of heavy menstrual bleeding [14-17]. However, the results of these studies remain limited and non-clinical.
Given the long history of traditional medicine in Iran, the growing demand for medicinal plants, and the ongoing studies on the effects of these plants on the treatment of heavy menstrual bleeding in Iran, no study has been found that systematically examines this body of research. Therefore, the present study aimed to systematically review clinical trials of herbal products on the severity of menstrual bleeding in order to help translate their results into clinical practice.
Information & Methods
This systematic review was conducted according to the recommendations of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement.
Search strategy
A search was conducted for all articles using clinical trial methods on the effectiveness of herbal compounds in the treatment of heavy menstrual bleeding, without time limits, until October 2024. Persian and English sources and the search engines Scopus, Web of Science, Cochrane, PubMed, IranMedex, SID, and Magiran were reviewed. Keywords based on MeSH, including Menstrual Bleeding, Herbal Medicine, Complementary Medicine, and Alternative Care, were used for the search. The AND and OR operators were employed in the search. These databases were searched without time limits until October 2024.
Inclusion criteria
Studies that included the following items were considered: study type—clinical trial; intervention type—prescription of herbal products for the treatment of heavy menstrual bleeding; outcomes—severity of menstrual bleeding, measurement of hemoglobin level, amount of bleeding, and number of pads used during menstruation; and published in Persian and English.
Exclusion criteria
Lack of access to the full text of articles, letters to the editor, commentaries, articles presented at conferences, preprints, retracted articles, theses, study protocols, review articles, and trials conducted on non-herbal products were excluded from the study.
All articles obtained from the aforementioned databases were checked for duplication in EndNote version 21 using the term “Duplicate,” and duplicate articles were removed. Then, the titles and abstracts of the articles obtained in the first stage, along with the full texts of the articles in the second stage, were reviewed separately by two researchers. Finally, articles that met the inclusion criteria were included in the study. Differences of opinion were resolved through discussion and exchange of views between the two authors.
Data extraction
Initially, a file was designed by the authors for data extraction. Then, the two authors independently reviewed the included articles based on the prepared file and extracted the data. The items in the prepared file included research characteristics, such as the first author, year of publication, study objective, study design, number of samples, study groups, intervention, outcome measurement method, study duration, and CONSORT checklist results. Any disagreements were resolved through discussion and exchange of opinions between the two researchers, after which the content was assessed for quality.
Quality assessment
The quality of the articles was assessed using the CONSORT 2018 checklist [12]. This checklist consists of 45 items that evaluate 7 sections. These sections include title, abstract, introduction, methods, findings, discussion, other information, and specialized sections. Selected articles received a score of one if they included the desired item in each section and a score of zero if they did not. The overall quality score of each article is calculated based on the sum of the CONSORT checklist items. Therefore, the highest score is 45, and the lowest score is zero.
Findings
Of the 28,108 articles from the initial search, 570 remained after removing duplicates. After reviewing the titles and abstracts of the articles and excluding irrelevant ones, 538 articles were screened for full text, and finally, 16 articles that met the inclusion criteria were included in the study (Figure 1).
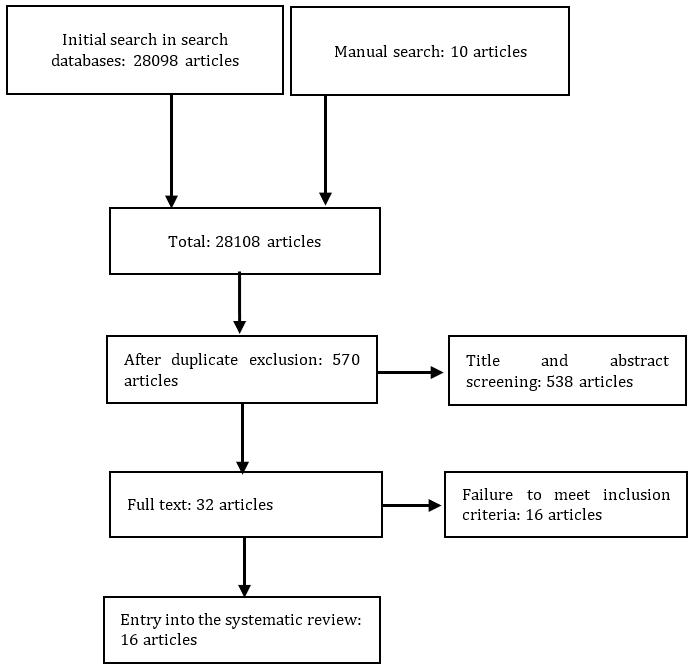
Figure 1. Article selection based on PRISMA
The publication date of the articles ranged from 2010 to 2024 and was conducted in Iran (100%). The total sample size across the articles was 1,333 people. The study design in all articles was a randomized clinical trial. The treatment process was examined using the Higham and Campbell, and Monga tables. The duration of the treatment process varied between 4 and 7 days. In 2 articles, the herbal product used was prepared in the form of drops, which were administered orally or topically on the abdomen at daily doses of 5 and 25 drops. In 12 articles, the product was used in the form of capsules, which were taken every 8 hours for 4 to 7 days during menstrual bleeding (Table 1).
Table 1. Summary of characteristics of articles included in the study
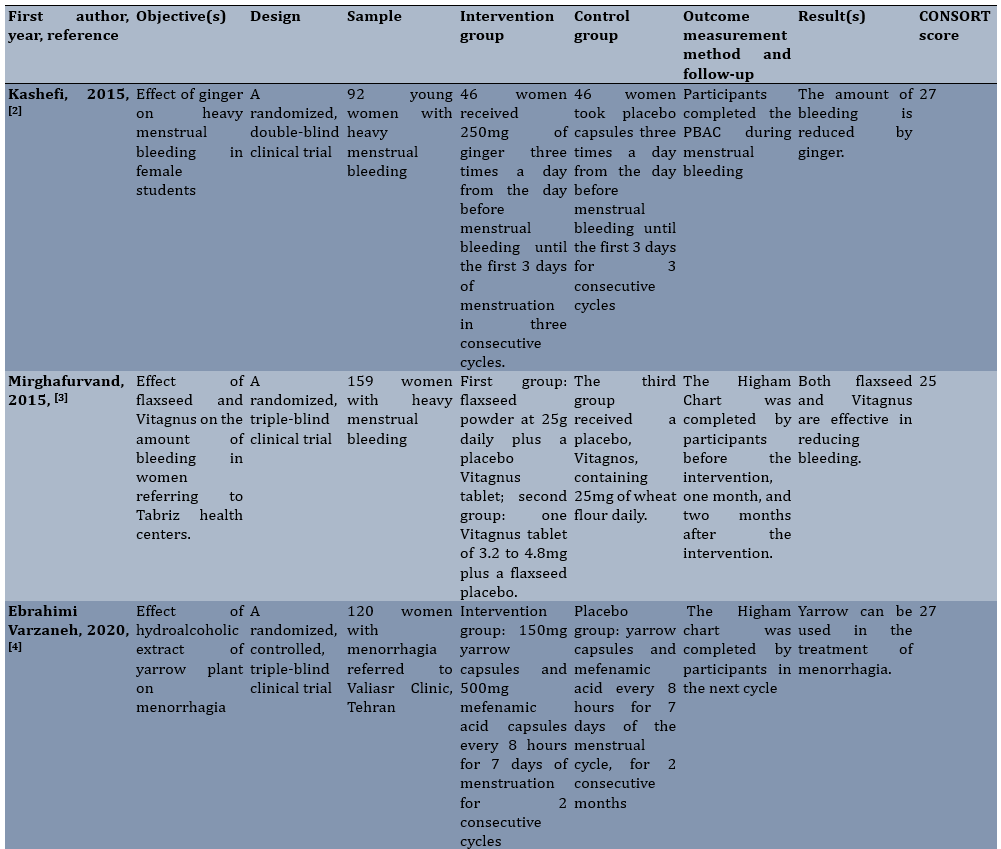
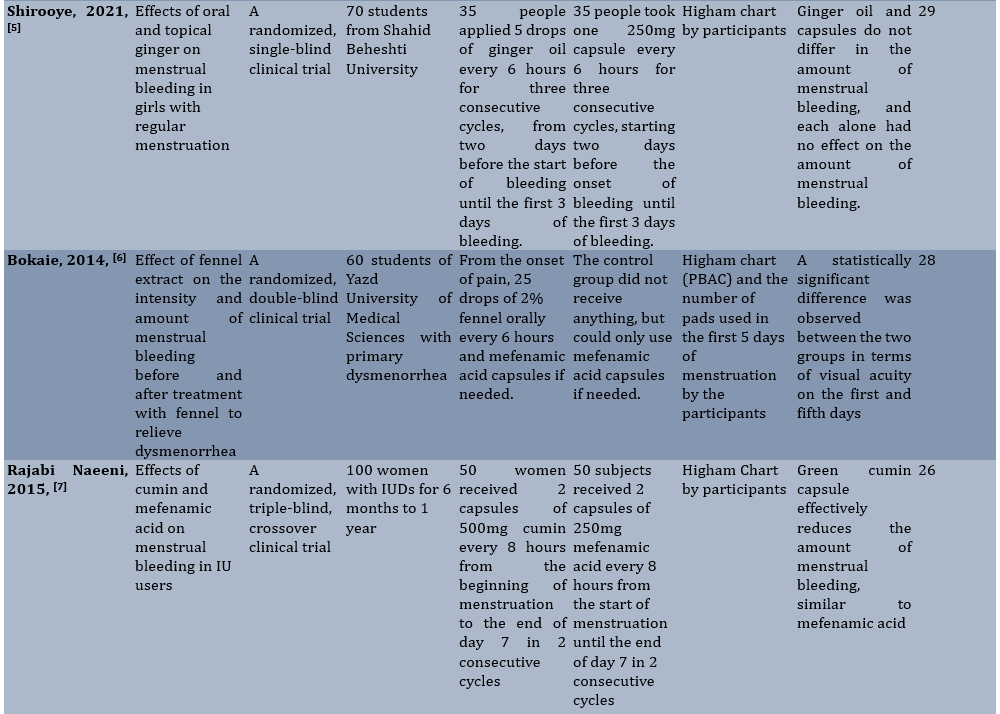
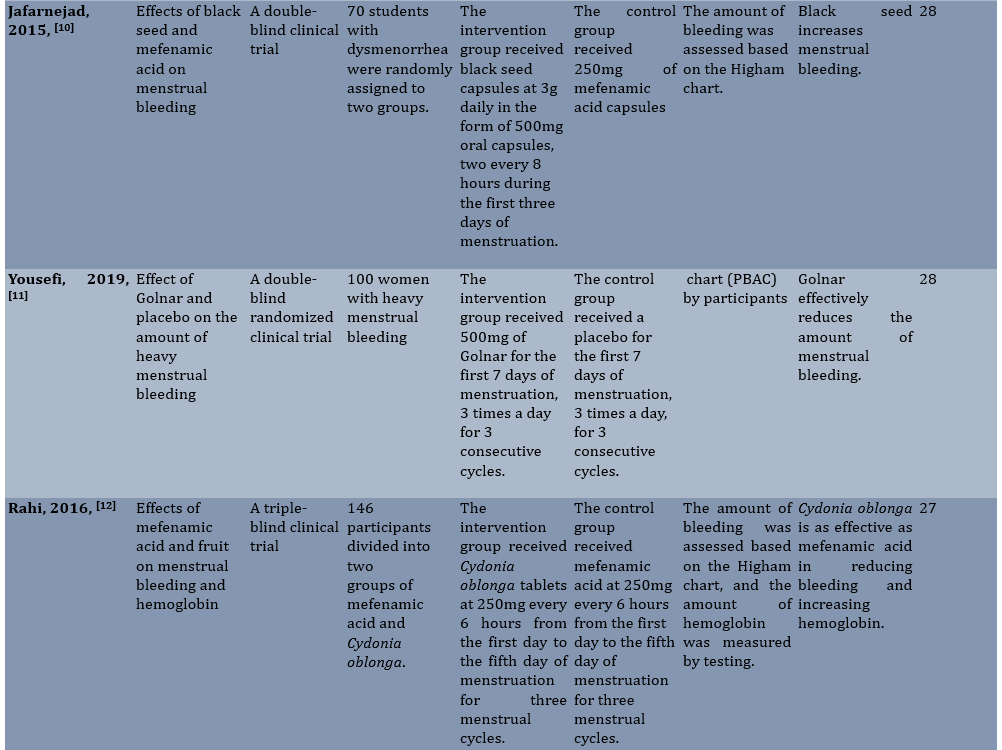
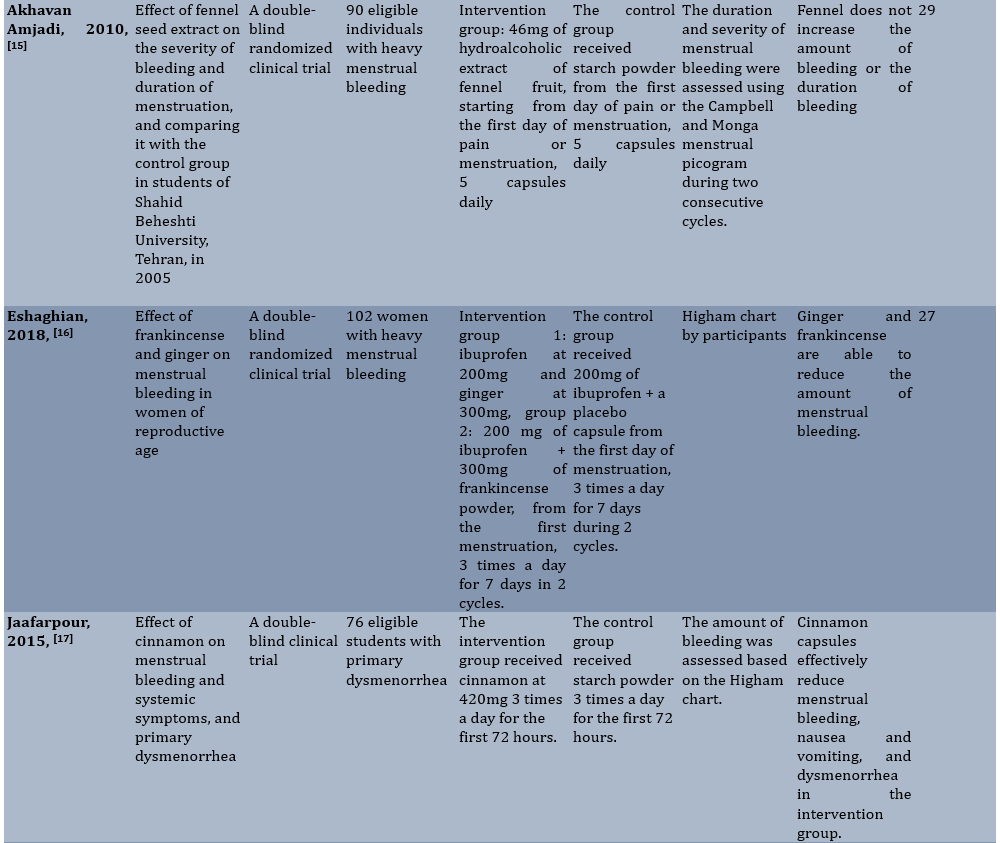
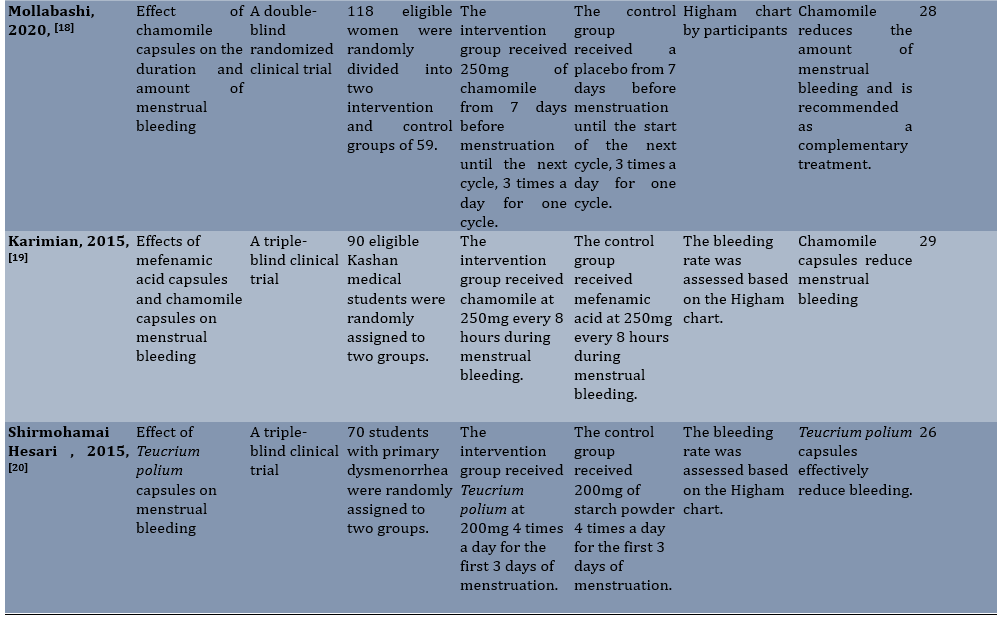
The quality of the articles assessed using the CONSORT statement ranged from 25 to 29, indicating a moderate quality of the articles. Due to the small number of clinical trial studies in this area, it was not possible to assess the risk of publication bias. There were two reviews in 2021 examining heavy and idiopathic bleeding, which have been studied in a smaller number of studies. However, this article examined the severity of bleeding in the normal menstrual cycle.
Herbal products studied for menstrual bleeding severity
In this section, herbs that have been used to treat heavy menstrual bleeding were reviewed, including flaxseed, yarrow, fennel, ginger, Cydonia oblonga, cumin, frankincense, cinnamon, plantain, chamomile, Golnar, black seed, and Teucrium polium. The products prepared from these herbs were used in the form of capsules and drops.
Linum usitotism
Flaxseed was studied in a research project for the management of heavy menstrual bleeding. This study was conducted as a triple-blind clinical trial involving 159 women. Subjects were randomly assigned to three groups of 53 participants each. The first group received 25 grams of flaxseed powder daily, the second group received one Vitagnus tablet daily (3.2 to 4.8mg), and the third group received a placebo for both drugs over 3 cycles. The Higham chart was completed by participants before the intervention and one and two months after the intervention. ANCOVA was used to analyze the data. The menstrual bleeding rate was significantly reduced in the first and second months after the intervention, such that the mean score of menstrual bleeding was significantly different in the first month after the intervention in the Vitagnus group [(4 - to 11.8 - confidence interval 95%) -7.9] compared to flaxseed [(5.6 - to 13.5 -) -9.6]. Additionally, in the second month after the intervention, the mean score in the Vitagnus group [(0.5 - to 15.2 -) -10.1] and [(2.5 - to -15.5) -10.4] was lower than that in the control group. No significant difference was observed between the Vitagnus and flaxseed groups. Both Vitagnus and flaxseed are effective in reducing bleeding [3].
Achillea millefolium
Yarrow was used in another study to reduce bleeding in individuals with menorrhagia. This study was conducted as a randomized, controlled, triple-blind clinical trial in 2016 involving 120 women with menorrhagia. The tools used included a demographic form, a Pectoral Bleeding Assessment Chart (PBAC), a scale, and a meter. After confirming menorrhagia in the baseline cycle, the intervention group was treated with 150mg of yarrow capsules and 500mg of mefenamic acid capsules, while the placebo group received yarrow and mefenamic acid placebo capsules every 8 hours for 7 days of the menstrual cycle for 2 consecutive months, followed by a PBAC chart assessment in the next cycle. Data analysis was performed using SPSS 19 with independent t-tests, paired t-tests, analysis of variance with repeated measures, and Friedman, Wilcoxon, Mann-Whitney, Fisher’s exact, and Chi-square tests. The duration and amount of menstrual bleeding were reduced in both groups; however, the reduction in the amount and duration of bleeding was greater in the yarrow group. Although the duration and amount of bleeding increased during the follow-up period after treatment in both groups compared to the intervention period, it remained less than before the intervention [4].
Foeniculum vulgare
A randomized clinical trial investigated the severity and amount of menstrual bleeding in fennel consumers among 59 students at Yazd University of Medical Sciences in 2014. The data collection tool was a questionnaire, and the severity of bleeding was measured by counting the pads used and using the PBAC chart. The data were evaluated using the Mann-Whitney U test, paired t-test, and independent t-test. The intervention group consumed 25 drops of 2% Foeniculum vulgare every 6 hours from the onset of pain. Because the subjects suffered from moderate to severe dysmenorrhea and double-blinding of the study was not possible due to the specific taste of fennel drops, ethical considerations allowed the subjects to use mefenamic acid capsules for pain relief. There was no statistically significant difference between the amount and severity of menstrual bleeding in the intervention group before and after the intervention (except for the first and fifth days), and also compared to the control group (except for the fifth day). Foeniculum vulgare can be used to relieve moderate to severe menstrual pain in individuals with moderate bleeding [7].
Another double-blind clinical trial assessed Foeniculum vulgare at Shahid Beheshti University of Medical Sciences in Tehran in 2005. In this study, 90 eligible subjects were enrolled and randomly assigned to two groups: an intervention group (46 participants) and a control group (44 participants). The drug was administered daily, with 5 capsules (2 in the morning, 2 in the afternoon, and 1 in the evening) during the first 3 days of menstruation, starting from the first day of pain or menstruation, and continued for two consecutive cycles until the subjects felt the need to take the drug. The duration and intensity of menstrual bleeding were determined based on the Campbell and Monga bleeding pyogram over the two consecutive cycles. SPSS version 10 software was used for data analysis, employing Friedman and Mann-Whitney U tests, as well as analysis of variance tests. Statistical tests did not show any significant difference in the intensity and duration of menstruation between the intervention and control groups. The Foeniculum vulgare extract did not increase the intensity of bleeding or the duration of menstruation [15].
Ginger
In a randomized, single-blind clinical trial conducted in 2016-2017 involving 70 students from Shahid Beheshti University of Medical Sciences, the effects of oral and topical ginger on menstrual bleeding were investigated. The subjects were divided into two groups of 35: one group received ginger capsules, and the other group received ginger oil. Both groups took the medication from 2 days before the onset of menstruation through the first 3 days of menstruation for 3 consecutive menstrual cycles. The PBAC chart was used to determine the amount of bleeding. Data analysis was performed using version 17 software, along with Mann-Whitney U and Friedman tests. The mean bleeding volume in the first cycle for the ginger capsule group was 104.91±64.01, which increased to 102.71±57.2 in the fourth cycle of intervention, and this change was not significant. In the ginger oil group, the mean bleeding volume in the first cycle was 92.8±43.46, while in the fourth cycle it was 102.88±71.14, showing no statistically significant difference. In this study, there was no difference between the ginger capsules and ginger oil regarding the amount of menstrual bleeding, and neither ginger oil nor ginger capsules alone were effective in reducing the amount of bleeding [5].
Another clinical trial of ginger for heavy menstrual bleeding was conducted in 2015 involving 92 eligible students. Both groups received ginger capsules and a placebo for three consecutive cycles. Bleeding was assessed using the PBAC score. In the ginger group, menstrual bleeding was significantly reduced. Ginger can be used to treat heavy menstrual bleeding [2].
Another clinical trial in 2014 assessed the effects of ginger on heavy menstrual bleeding in 92 college students who met the clinical criteria. Participants were randomly divided into two groups of 46. The intervention group received capsules containing 250mg of ginger powder three times a day from one day before menstruation through the first three days of menstruation, while the control group received capsules containing a placebo three times a day during the same period. Both groups were followed for 6 cycles. During the study, participants used sanitary pads and were assessed with a Higham chart. Ultimately, after statistical analysis, ginger was found to effectively reduce the amount of menstrual bleeding in the participants [6].
Cydonia oblonga
A 2016 randomized, triple-blind clinical trial studied the effects of fenugreek and mefenamic acid on menstrual bleeding in 146 participants. Seventy-two individuals in the intervention group received 250mg of fenugreek in tablet form every 6 hours from the first day of menstruation to the fifth day for three menstrual cycles. In the control group, 74 subjects were prescribed 250mg of mefenamic acid every 6 hours from the first day of menstruation to the fifth day for three menstrual cycles. Menstrual bleeding in the participants was also examined based on the Higham chart and hemoglobin levels. After analysis, it was determined that fenugreek was as effective as mefenamic acid in reducing menstrual bleeding and increasing hemoglobin levels [12].
Cuminum cyminum
A randomized, triple-blind, crossover clinical trial investigated the effects of cumin and mefenamic acid on menstrual bleeding in 100 IUD users referred to 6 health centers in Karaj. This study was conducted in three stages. In the first stage, the menstrual bleeding rate of all samples was measured during one cycle using the Higham chart. In the second stage, subjects were randomly divided into two groups: one receiving mefenamic acid and the other receiving cumin, and they received the capsules during two consecutive cycles. In the third stage, the treatment method of the opposite group was repeated for each participant by switching the drugs for two more consecutive cycles. The amount of bleeding and the duration of menstruation were measured during these 5 cycles using a Higham device. Considering that the maximum effect duration of cumin is 24 hours and that of mefenamic acid capsules is 6 to 8 hours, its use on the 7th day of menstruation will not affect subsequent cycles. The mean menstrual bleeding score before treatment was 154.26±60.08, which decreased to 106.68±45.38 in the mefenamic acid group and 105.8±40.56 in the cumin group after the intervention, indicating a significant reduction. This study showed that cumin capsules can effectively reduce menstrual bleeding similarly to mefenamic acid [7].
Frankincense and Ginger
A randomized clinical trial studied the effects of ginger and frankincense on heavy menstrual bleeding. In this study, 102 patients were divided into three groups. All patients received 200mg of ibuprofen, along with 300mg of frankincense, 300mg of ginger, and a placebo that resembled the other two drugs. Patients took the medications three times a day for 7 days during their menstrual cycle, starting on the first day of menstruation and continuing for two cycles. The duration of menstrual bleeding was reduced in both the frankincense and ginger groups, but there was no significant difference in the placebo group. The amount of menstrual bleeding decreased in all groups, but there was no statistically significant difference between the groups. Quality of life also improved in both the ginger and frankincense groups, while no change was observed in the placebo group. According to the results of this study, frankincense and ginger appear to be effective complementary treatments for heavy menstrual bleeding [16].
Cinnamon
A randomized, double-blind, controlled clinical trial was conducted on 76 female students. Thirty-eight subjects received a placebo in the form of starch capsules three times a day, while 38 subjects received capsules containing 420mg of cinnamon three times a day. Pain and nausea were assessed using a visual analogue scale, and bleeding was measured using pads. Parameters were assessed during the first 72 hours of the cycle. The average amount of bleeding in the cinnamon group was significantly reduced compared to the placebo group. The level of pain in the cinnamon group was also lower than in the placebo group. Additionally, the incidence of nausea and vomiting in the cinnamon group was significantly reduced compared to the placebo group. Therefore, cinnamon was able to significantly reduce pain, nausea, and vomiting, as well as the amount of menstrual bleeding, without side effects [17].
Plantain
In a 2019 randomized, double-blind, placebo-controlled clinical trial conducted in Mashhad, 68 women aged 36 to 45 years who had heavy menstrual bleeding participated. The intervention group received placebo capsules and plantain syrup, while the control group received mefenamic acid capsules and placebo syrup during the first 5 days of the menstrual cycle for three consecutive cycles. Patients were asked about bleeding one month before the intervention, and hemoglobin levels were measured at the beginning and end of the study. The amount and duration of menstruation decreased in both groups. There was no statistically significant difference between the two groups in the severity of bleeding; however, the duration of bleeding was significantly reduced in the mefenamic acid group compared to the plantain group. Although there was a statistically significant difference in hemoglobin levels in the mefenamic acid group before and after the intervention, there was no statistically significant difference in hemoglobin levels between the two groups after the intervention. Therefore, plantain syrup can be used as a complementary treatment for heavy menstrual bleeding [13].
Chamomile
A double-blind clinical trial was conducted in 2020 involving 118 students at Guilan University of Medical Sciences. The participants were divided into two groups of 59. The intervention group took 250mg chamomile capsules three times a day, while the placebo group took a placebo three times a day, starting 7 days before the onset of menstrual bleeding. A Higham chart was used to assess the amount of blood loss during menstruation. Data were analyzed using SPSS version 20. The amount of bleeding was reduced in the chamomile group. Although statistical tests did not show a statistically significant difference in the duration and interval between two bleedings, chamomile can reduce the amount of bleeding during menstruation and can be used as a treatment method [13].
Another randomized, triple-blind clinical study was conducted in 2011 involving 90 participants in Kashan. The participants were randomly assigned to two groups: mefenamic acid and chamomile. Forty-five individuals were given mefenamic acid capsules every 8 hours, while the other 45 received 250mg chamomile capsules every 8 hours during two consecutive menstrual cycles. A Higham chart was used to determine bleeding. Data analysis was performed using SPSS version 16 software, along with the Chi-square test, Fisher’s t-test, and paired t-test. The amount of bleeding in the two treatment groups showed a statistically significant decrease compared to before treatment. In the comparison between the two drugs, the difference was not statistically significant; however, the reduction in bleeding due to chamomile and mefenamic acid in the second cycle was not different from that in the first cycle. Taking chamomile capsules can reduce menstrual bleeding and can be recommended for the treatment of heavy menstrual bleeding [18].
Golnar
A randomized, double-blind clinical trial was conducted in Qom in 2017 involving 100 participants. The participants were divided into two groups of 50. The intervention group received 500mg Golnar capsules during the first 7 days of the menstrual cycle for three consecutive cycles, while the placebo group received placebo capsules in the same manner. Bleeding duration and volume were assessed using the Higham chart, quality of life was assessed using the McGill Quality of Life Questionnaire, and hemoglobin levels were measured for 3 months. At the end of the study, 82 participants (43 in the Golnar group and 39 in the placebo group) were evaluated over the 3 months. In the Golnar group, bleeding rates were reduced, and quality of life improved, while the changes in the placebo group were not significant. Hemoglobin levels increased in the Golnar group and decreased in the placebo group. Golnar is effective for individuals who experience heavy bleeding, and it is suggested that a study with a larger sample size be conducted to investigate potential side effects [11].
Nigella
A double-blind clinical trial was conducted in 2014 involving 70 individuals at Mashhad University of Medical Sciences. The subjects were randomly assigned to the mefenamic acid and black seed groups. The study was conducted in two stages. First, all participants were screened for bleeding over two cycles. Then, each participant was randomly assigned either mefenamic acid capsules or black seed capsules for two consecutive cycles. The first group received 3 grams of black seed capsules orally daily (two 500mg capsules every 8 hours), while the second group received 250mg of mefenamic acid every 8 hours for the first 3 days of menstruation. The Hegam chart was used to assess the amount of bleeding. Data were analyzed using SPSS version 16, along with the independent t-test and the Friedman test. The mean bleeding rate in the black seed group before the intervention was 85.20±37.85, which increased to 85.62 ± 34.20 in the first treatment cycle and to 83.77±31.81 in the second treatment cycle. In the mefenamic acid group, the mean bleeding rate before the intervention was 83.77±38.31, which decreased to 78.05±32.66 in the first treatment cycle and to 76.75±29.71 in the second treatment cycle. There was no statistically significant difference between the two groups in terms of bleeding rates in the first and second cycles of treatment. Black seed can increase menstrual bleeding, but this increase was not statistically significant compared to mefenamic acid [10].
Teucrium polium
In a triple-blind clinical trial conducted in 2015 involving 70 students with primary dysmenorrhea, the effect of Teucrium polium on the duration of menstrual bleeding was investigated. The students were randomly divided into two groups of 35, with one group receiving Teucrium polium capsules and the other receiving placebo capsules. The first group was prescribed capsules containing 200mg of Teucrium polium extract four times a day during the first three days of menstruation, while the placebo group was prescribed 200mg starch-containing capsules in the same manner. The McGill Pain Questionnaire (MPQ) was used to collect data, and a questionnaire was used to assess the duration of menstrual bleeding. Data were analyzed using SPSS version 20 software, employing independent t-tests, the Mann-Whitney U test, and repeated measures ANOVA. The mean duration of menstrual bleeding before drug administration was 6.3(1.1) days in the Teucrium polium group and 6.5(2.6) days in the placebo group, with no significant difference between the two groups. The duration of menstrual bleeding in the Teucrium polium treatment group was significantly reduced compared to before treatment; however, there was no significant difference in the placebo group. Teucrium polium was more effective than a placebo in reducing menstrual bleeding. The use of Teucrium polium is recommended for the treatment of heavy menstrual bleeding and the prevention of subsequent iron deficiency anemia in women [20].
Discussion
This study aimed to systematically review clinical trials of herbal products on the severity of menstrual bleeding. Herbal remedies are part of traditional medicine. In recent years, there has been a trend toward using herbal supplements in the treatment of diseases worldwide. It is generally believed that herbal medicines are effective and have fewer side effects than chemical drugs. Many types of plants are used for female disorders, such as irregular menstrual cycles and heavy menstrual bleeding [1, 20]. Some studies have shown that certain herbal remedies are effective in reducing menstrual bleeding [13]. Calamus, black seed, marigold, chamomile, ginger, cumin, plantain, cinnamon, frankincense, fennel, yarrow, and flaxseed have been studied, and all, except for black seed, have been effective in treating heavy menstrual bleeding. Among the herbs studied, ginger, fennel, and chamomile were examined in two studies, where chamomile showed little effect on reducing menstrual bleeding, and ginger was effective in reducing bleeding in one study but not in another. In a study conducted on black seed, it was found that black seed increased menstrual bleeding, and the number of studies on other herbs was limited. Therefore, a precise conclusion and interpretation of the results of the studies cannot be drawn.
One of the plants studied is flaxseed. In a study, flaxseed powder was used. Flaxseed is the richest source of lignans, which are one of the main classes of phytoestrogens. This plant contains the essential fatty acid α-linolenic acid, which is a biological precursor to omega-3, and it also contains fiber. Lignans function as both estrogen agonists and antagonists and possess antioxidant properties. Flaxseed and lignans may have potent antiestrogenic effects on estrogen receptors. Phytoestrogens derived from flaxseed protect female reproductive tissues (such as the breast and uterus) from excessive estrogen stimulation [3].
Another plant studied in this research was yarrow. Yarrow contains inulin, phytosterols, acyl-leic acid, alkaloids, flavonoids, sesquiterpenes, oxalic acid, choline, resin, polyphenolic compounds, lactones, and tannins. This plant has antiseptic, antispasmodic, analgesic, anti-inflammatory, antioxidant, anticancer, diuretic, and estrogenic activities. Yarrow is used as an astringent for menstrual disorders, as a blood-thinning agent, as a blood-clotting agent, and as a treatment for bleeding. It has also been historically used to stop internal bleeding [4]. Yarrow contains substances, such as flavonoids, sesquiterpenes, and tannins that act as uterine smooth muscle contractants and have anti-inflammatory and antioxidant effects, which are effective in reducing severe menstrual bleeding [21].
Another plant studied in this research was Foeniculum vulgare. The parts used were the roots, leaves, and fruit, which have anti-inflammatory and antispasmodic effects. Fennel is rich in phytoestrogens, including lignans and isoflavones. The plant exhibits analgesic and antispasmodic effects on spasms caused by oxytocin and prostaglandins, and it facilitates the release of menstrual blood in a shorter period of time [6, 22].
Another plant examined was ginger. Ginger is a plant used for many disorders, such as dysmenorrhea, nausea caused by pregnancy, and skin inflammation. The anti-inflammatory effects of ginger are attributed to the modulation of prostaglandin synthesis and increased uterine smooth muscle activity. Ginger contains fat, carbohydrates, protein, fiber, water, volatile oil, monoterpenoids, sesquiterpenoids, camphene, and borneol [5]. The effect of ginger on reducing menstrual bleeding may be due to an increase in the levels of endometrial prostaglandins, such as prostaglandin F2α, prostaglandin E, and prostacyclin, which can reduce bleeding by contracting the uterine muscles. A few other studies have shown that platelet aggregation during menstrual bleeding increases with ginger consumption [2, 16].
Another studied plant was cumin. It is effective in muscle contractions and contains compounds such as carotenoids, myrcene, limonene, alpha-pinene, and beta-pinene. Studies have shown that alpha- and beta-pinene have anti-inflammatory properties, while carotenoids and limonene counteract the effects of prostaglandins. In traditional medicine, its mixture with olive oil, when applied vaginally, prevents heavy menstrual bleeding. Cumin appears to have a dual role in regulating menstruation, being effective in both treating amenorrhea and reducing menstrual bleeding [7].
Another herb studied was frankincense. In this study, frankincense and ginger were compared, and both were found to reduce menstrual bleeding. Frankincense contains boswellic acid and other five-ring triterpenes, which have a chemical structure similar to steroids. This plant is used in various countries as an anti-inflammatory, analgesic, and anti-arthritic herbal medicine, for the treatment of allergies, bronchitis, tumors, wounds, fever, diarrhea, vomiting, memory enhancement, and other conditions. Frankincense is also recommended for the treatment of eye diseases and the prevention of intestinal bleeding. However, the mechanism by which frankincense reduces bleeding has not been mentioned in studies [23].
Cinnamon was another herb studied. Cinnamon was able to significantly reduce pain, nausea, vomiting, and menstrual bleeding without any side effects. Cinnamon is an herb that has anti-inflammatory and antimicrobial properties. It contains coumarin, cinnamyl acetate, hydroxycinnamaldehyde, cinnamaldehyde, and N-acetyl-L-cysteine. These compounds belong to the benzopyrone group and are found in cinnamon, green tea, and peppermint. Cinnamon is used to treat depression, rheumatism, and muscle pain [23, 24]. According to reviews conducted in various studies, the mechanism of action of cinnamon is not mentioned.
Plantain is another plant that was studied in this research. It is used to treat conditions such as colds, wounds, fever, bleeding, and inflammation. Plantain is one of the best medicines used both orally and vaginally to reduce menstrual bleeding. The medicinal properties of this plant include antifungal, analgesic, antihemorrhagic, anti-inflammatory, phytoestrogenic, androgenic, and anemic effects. It was also able to effectively reduce menstrual bleeding [13].
Chamomile was investigated in this study. Research has shown that this plant possesses hemostatic, antiseptic, and sedative properties. Chamomile also has anti-inflammatory activity, which is attributed to compounds such as matricin (a plant alkaloid), bisabolol (a plant alkaloid), and their oxides. Chamomile contains chamazulene, which has anti-inflammatory and antioxidant effects, as well as apigenin (anti-inflammatory, sedative, and antineoplastic), flavonoids (anti-inflammatory and anti-anxiety), alpha-bisabolol (anti-inflammatory and digestive effects), alpha-heteroside, beta-heteroside, and methoxycoumarin. Additionally, chamomile has a strong antispasmodic effect. Glycine has also been found in chamomile, which can relieve uterine spasms and relax the uterus [19, 18].
Another studied plant was Golnar. Golnar is composed of six plant components, including pomegranate flowers, Persian Golnar from the family Hanaeaceae (the main component), acacia or gum arabic, clay (a compound of iron oxide), rose, tragacanth, and cinnamon oil. Golnar has an inhibitory effect on prostaglandin synthesis. Memarzadeh et al. examined the effect of pomegranate on menstrual bleeding, finding that the amount of bleeding decreases, which is consistent with this study. Golnar contains cinnamon oil, which includes tannins that have astringent properties [11].
Black seed was another studied plant. The part used in black seed is its seed, the physiological effect of which is related to the volatile oil that contains the active ingredient thymoquinone. Black seed has many properties, including antibacterial, analgesic, smooth muscle relaxant, antioxidant, anti-inflammatory, antihistamine, and protective effects on the kidney, liver, and cardiovascular tissues, as well as promoting bile and uric acid excretion and lowering sugar, fat, and blood pressure. The relaxing and antispasmodic effects of black seed have been proven in studies [10].
Teucrium polium was the last plant examined. The medicinal use of Teucrium polium dates back to the time of Hippocrates and Galen. It has a tonic and anticonvulsant effect, and its use is beneficial for treating diseases of the genitourinary system and delaying or preventing pregnancy. Studies have investigated the anti-contractile effect of Teucrium polium on the uterus. Teucrium polium, by possessing adrenergic agonist properties and increasing cAMP, causes uterine relaxation. Research conducted on Teucrium polium has shown that the plant contains tannins, triterpenoids, saponins, sterols, flavonoids, glycosides, alpha and beta pinene, and leucoanthocyanins [8, 20].
Although the results showed that these herbs have positive effects in treating heavy menstrual bleeding, the number of studies on each product is limited, making it difficult to reach a scientific and accurate decision. Therefore, better-designed studies are needed to investigate the effects of these herbs and compare their different dosage forms and dosages. Also, the mechanism of action of each of these herbs has been obtained in laboratory studies and requires further investigation in a clinical setting. Therefore, the mechanism of action of these herbs on the treatment of heavy menstrual bleeding may have differences that require further investigation and study.
These plants can affect the severity of menstrual bleeding, and although studies showed that each of these plants has different active ingredients and affects the process of reducing menstrual bleeding through different mechanisms, these plants also have common properties, such as anti-inflammatory, antibacterial, and antioxidant properties.
Conclusion
The studied plants are effective in treating heavy menstrual bleeding.
Acknowledgments: The authors would like to sincerely thank their colleagues who helped them with their advice and knowledge in writing the paper.
Ethical Permissions: Nothing declared by the authors.
Conflicts of Interests: The authors have no conflicts of interest to declare.
Authors' Contribution: Goudarzi F (First author), Introduction author/Methodologist/Main researcher/Discussion author (50%); Hekmatzadeh SF. (Second author), Introduction author/Methodologist/Assistant researcher/Statistical analyst/ Discussion author (50%);
Funding/Support: This study was supported by the Yasuj University of Medical Sciences.
Heavy menstrual bleeding is a common problem in women that negatively impacts their lifestyle. It is known by terms such as menorrhagia, hypermenorrhea, abnormal uterine bleeding, bleeding due to abnormal uterine function, and excessive uterine bleeding. It is defined as blood loss of more than 80 ml per cycle or a bleeding duration of more than seven days [1]. Between 5% and 29% of women’s visits to the hospital are for heavy menstrual bleeding. Excessive bleeding can interfere with work, daily activities, and social participation. It may also lead to iron deficiency anemia in women. Studies have reported that 18 million young women in the United States have iron deficiency anemia due to heavy bleeding [2]. Anemia can cause complications such as weakness, fatigue, unexplained weight loss, mood swings, and cognitive impairment [3].
Laboratory tests have identified two primary factors in heavy bleeding as excessive fibrinolysis and imbalanced prostaglandin levels [2]. The causes of menorrhagia include hormonal, mechanical, and coagulation disorders, and risk factors include age, racial and cultural groups, number of deliveries, and lifestyle [4]. Many treatments have been proposed for heavy menstrual bleeding, including birth control pills, oral progestins, tranexamic acid, and nonsteroidal anti-inflammatory drugs. Although these drugs may be effective, they have side effects [2].
Surgical procedures include fibroid removal, myomectomy, uterine artery embolization, endometrial ablation, and hysterectomy. These procedures have complications, including repeated treatments, potential serious complications, patient discomfort, and cost; thus, it is essential to have appropriate treatment methods that have minimal side effects and are acceptable to the patient [4]. Therefore, the tendency to use medicinal plants for the treatment of diseases has increased in recent decades [2].
Women have a particular inclination to use herbal medicines for treating diseases and frequently use these remedies to address problems, such as dysmenorrhea, relief of menopausal symptoms, menstrual disorders, mood disorders, prevention of osteoporosis, and issues during pregnancy [5]. Herbal remedies, such as ginger (Zingiber officinale) [2, 5], yarrow (Achillea millefolium) [4], fennel (Foeniculum vulgare) [6], flaxseed (Linum usitatissimum) [3], cumin (Cuminum cyminum) [7], Teucrium polium [8], nettle (Urtica dioica) [9], black seed (Nigella sativa) [10], Golnar (Punica granatum) [11], Cydonia oblonga [12], and chamomile (Matricaria chamomilla) [13] have been used in the treatment of heavy menstrual bleeding [14-17]. However, the results of these studies remain limited and non-clinical.
Given the long history of traditional medicine in Iran, the growing demand for medicinal plants, and the ongoing studies on the effects of these plants on the treatment of heavy menstrual bleeding in Iran, no study has been found that systematically examines this body of research. Therefore, the present study aimed to systematically review clinical trials of herbal products on the severity of menstrual bleeding in order to help translate their results into clinical practice.
Information & Methods
This systematic review was conducted according to the recommendations of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement.
Search strategy
A search was conducted for all articles using clinical trial methods on the effectiveness of herbal compounds in the treatment of heavy menstrual bleeding, without time limits, until October 2024. Persian and English sources and the search engines Scopus, Web of Science, Cochrane, PubMed, IranMedex, SID, and Magiran were reviewed. Keywords based on MeSH, including Menstrual Bleeding, Herbal Medicine, Complementary Medicine, and Alternative Care, were used for the search. The AND and OR operators were employed in the search. These databases were searched without time limits until October 2024.
Inclusion criteria
Studies that included the following items were considered: study type—clinical trial; intervention type—prescription of herbal products for the treatment of heavy menstrual bleeding; outcomes—severity of menstrual bleeding, measurement of hemoglobin level, amount of bleeding, and number of pads used during menstruation; and published in Persian and English.
Exclusion criteria
Lack of access to the full text of articles, letters to the editor, commentaries, articles presented at conferences, preprints, retracted articles, theses, study protocols, review articles, and trials conducted on non-herbal products were excluded from the study.
All articles obtained from the aforementioned databases were checked for duplication in EndNote version 21 using the term “Duplicate,” and duplicate articles were removed. Then, the titles and abstracts of the articles obtained in the first stage, along with the full texts of the articles in the second stage, were reviewed separately by two researchers. Finally, articles that met the inclusion criteria were included in the study. Differences of opinion were resolved through discussion and exchange of views between the two authors.
Data extraction
Initially, a file was designed by the authors for data extraction. Then, the two authors independently reviewed the included articles based on the prepared file and extracted the data. The items in the prepared file included research characteristics, such as the first author, year of publication, study objective, study design, number of samples, study groups, intervention, outcome measurement method, study duration, and CONSORT checklist results. Any disagreements were resolved through discussion and exchange of opinions between the two researchers, after which the content was assessed for quality.
Quality assessment
The quality of the articles was assessed using the CONSORT 2018 checklist [12]. This checklist consists of 45 items that evaluate 7 sections. These sections include title, abstract, introduction, methods, findings, discussion, other information, and specialized sections. Selected articles received a score of one if they included the desired item in each section and a score of zero if they did not. The overall quality score of each article is calculated based on the sum of the CONSORT checklist items. Therefore, the highest score is 45, and the lowest score is zero.
Findings
Of the 28,108 articles from the initial search, 570 remained after removing duplicates. After reviewing the titles and abstracts of the articles and excluding irrelevant ones, 538 articles were screened for full text, and finally, 16 articles that met the inclusion criteria were included in the study (Figure 1).

Figure 1. Article selection based on PRISMA
The publication date of the articles ranged from 2010 to 2024 and was conducted in Iran (100%). The total sample size across the articles was 1,333 people. The study design in all articles was a randomized clinical trial. The treatment process was examined using the Higham and Campbell, and Monga tables. The duration of the treatment process varied between 4 and 7 days. In 2 articles, the herbal product used was prepared in the form of drops, which were administered orally or topically on the abdomen at daily doses of 5 and 25 drops. In 12 articles, the product was used in the form of capsules, which were taken every 8 hours for 4 to 7 days during menstrual bleeding (Table 1).
Table 1. Summary of characteristics of articles included in the study





The quality of the articles assessed using the CONSORT statement ranged from 25 to 29, indicating a moderate quality of the articles. Due to the small number of clinical trial studies in this area, it was not possible to assess the risk of publication bias. There were two reviews in 2021 examining heavy and idiopathic bleeding, which have been studied in a smaller number of studies. However, this article examined the severity of bleeding in the normal menstrual cycle.
Herbal products studied for menstrual bleeding severity
In this section, herbs that have been used to treat heavy menstrual bleeding were reviewed, including flaxseed, yarrow, fennel, ginger, Cydonia oblonga, cumin, frankincense, cinnamon, plantain, chamomile, Golnar, black seed, and Teucrium polium. The products prepared from these herbs were used in the form of capsules and drops.
Linum usitotism
Flaxseed was studied in a research project for the management of heavy menstrual bleeding. This study was conducted as a triple-blind clinical trial involving 159 women. Subjects were randomly assigned to three groups of 53 participants each. The first group received 25 grams of flaxseed powder daily, the second group received one Vitagnus tablet daily (3.2 to 4.8mg), and the third group received a placebo for both drugs over 3 cycles. The Higham chart was completed by participants before the intervention and one and two months after the intervention. ANCOVA was used to analyze the data. The menstrual bleeding rate was significantly reduced in the first and second months after the intervention, such that the mean score of menstrual bleeding was significantly different in the first month after the intervention in the Vitagnus group [(4 - to 11.8 - confidence interval 95%) -7.9] compared to flaxseed [(5.6 - to 13.5 -) -9.6]. Additionally, in the second month after the intervention, the mean score in the Vitagnus group [(0.5 - to 15.2 -) -10.1] and [(2.5 - to -15.5) -10.4] was lower than that in the control group. No significant difference was observed between the Vitagnus and flaxseed groups. Both Vitagnus and flaxseed are effective in reducing bleeding [3].
Achillea millefolium
Yarrow was used in another study to reduce bleeding in individuals with menorrhagia. This study was conducted as a randomized, controlled, triple-blind clinical trial in 2016 involving 120 women with menorrhagia. The tools used included a demographic form, a Pectoral Bleeding Assessment Chart (PBAC), a scale, and a meter. After confirming menorrhagia in the baseline cycle, the intervention group was treated with 150mg of yarrow capsules and 500mg of mefenamic acid capsules, while the placebo group received yarrow and mefenamic acid placebo capsules every 8 hours for 7 days of the menstrual cycle for 2 consecutive months, followed by a PBAC chart assessment in the next cycle. Data analysis was performed using SPSS 19 with independent t-tests, paired t-tests, analysis of variance with repeated measures, and Friedman, Wilcoxon, Mann-Whitney, Fisher’s exact, and Chi-square tests. The duration and amount of menstrual bleeding were reduced in both groups; however, the reduction in the amount and duration of bleeding was greater in the yarrow group. Although the duration and amount of bleeding increased during the follow-up period after treatment in both groups compared to the intervention period, it remained less than before the intervention [4].
Foeniculum vulgare
A randomized clinical trial investigated the severity and amount of menstrual bleeding in fennel consumers among 59 students at Yazd University of Medical Sciences in 2014. The data collection tool was a questionnaire, and the severity of bleeding was measured by counting the pads used and using the PBAC chart. The data were evaluated using the Mann-Whitney U test, paired t-test, and independent t-test. The intervention group consumed 25 drops of 2% Foeniculum vulgare every 6 hours from the onset of pain. Because the subjects suffered from moderate to severe dysmenorrhea and double-blinding of the study was not possible due to the specific taste of fennel drops, ethical considerations allowed the subjects to use mefenamic acid capsules for pain relief. There was no statistically significant difference between the amount and severity of menstrual bleeding in the intervention group before and after the intervention (except for the first and fifth days), and also compared to the control group (except for the fifth day). Foeniculum vulgare can be used to relieve moderate to severe menstrual pain in individuals with moderate bleeding [7].
Another double-blind clinical trial assessed Foeniculum vulgare at Shahid Beheshti University of Medical Sciences in Tehran in 2005. In this study, 90 eligible subjects were enrolled and randomly assigned to two groups: an intervention group (46 participants) and a control group (44 participants). The drug was administered daily, with 5 capsules (2 in the morning, 2 in the afternoon, and 1 in the evening) during the first 3 days of menstruation, starting from the first day of pain or menstruation, and continued for two consecutive cycles until the subjects felt the need to take the drug. The duration and intensity of menstrual bleeding were determined based on the Campbell and Monga bleeding pyogram over the two consecutive cycles. SPSS version 10 software was used for data analysis, employing Friedman and Mann-Whitney U tests, as well as analysis of variance tests. Statistical tests did not show any significant difference in the intensity and duration of menstruation between the intervention and control groups. The Foeniculum vulgare extract did not increase the intensity of bleeding or the duration of menstruation [15].
Ginger
In a randomized, single-blind clinical trial conducted in 2016-2017 involving 70 students from Shahid Beheshti University of Medical Sciences, the effects of oral and topical ginger on menstrual bleeding were investigated. The subjects were divided into two groups of 35: one group received ginger capsules, and the other group received ginger oil. Both groups took the medication from 2 days before the onset of menstruation through the first 3 days of menstruation for 3 consecutive menstrual cycles. The PBAC chart was used to determine the amount of bleeding. Data analysis was performed using version 17 software, along with Mann-Whitney U and Friedman tests. The mean bleeding volume in the first cycle for the ginger capsule group was 104.91±64.01, which increased to 102.71±57.2 in the fourth cycle of intervention, and this change was not significant. In the ginger oil group, the mean bleeding volume in the first cycle was 92.8±43.46, while in the fourth cycle it was 102.88±71.14, showing no statistically significant difference. In this study, there was no difference between the ginger capsules and ginger oil regarding the amount of menstrual bleeding, and neither ginger oil nor ginger capsules alone were effective in reducing the amount of bleeding [5].
Another clinical trial of ginger for heavy menstrual bleeding was conducted in 2015 involving 92 eligible students. Both groups received ginger capsules and a placebo for three consecutive cycles. Bleeding was assessed using the PBAC score. In the ginger group, menstrual bleeding was significantly reduced. Ginger can be used to treat heavy menstrual bleeding [2].
Another clinical trial in 2014 assessed the effects of ginger on heavy menstrual bleeding in 92 college students who met the clinical criteria. Participants were randomly divided into two groups of 46. The intervention group received capsules containing 250mg of ginger powder three times a day from one day before menstruation through the first three days of menstruation, while the control group received capsules containing a placebo three times a day during the same period. Both groups were followed for 6 cycles. During the study, participants used sanitary pads and were assessed with a Higham chart. Ultimately, after statistical analysis, ginger was found to effectively reduce the amount of menstrual bleeding in the participants [6].
Cydonia oblonga
A 2016 randomized, triple-blind clinical trial studied the effects of fenugreek and mefenamic acid on menstrual bleeding in 146 participants. Seventy-two individuals in the intervention group received 250mg of fenugreek in tablet form every 6 hours from the first day of menstruation to the fifth day for three menstrual cycles. In the control group, 74 subjects were prescribed 250mg of mefenamic acid every 6 hours from the first day of menstruation to the fifth day for three menstrual cycles. Menstrual bleeding in the participants was also examined based on the Higham chart and hemoglobin levels. After analysis, it was determined that fenugreek was as effective as mefenamic acid in reducing menstrual bleeding and increasing hemoglobin levels [12].
Cuminum cyminum
A randomized, triple-blind, crossover clinical trial investigated the effects of cumin and mefenamic acid on menstrual bleeding in 100 IUD users referred to 6 health centers in Karaj. This study was conducted in three stages. In the first stage, the menstrual bleeding rate of all samples was measured during one cycle using the Higham chart. In the second stage, subjects were randomly divided into two groups: one receiving mefenamic acid and the other receiving cumin, and they received the capsules during two consecutive cycles. In the third stage, the treatment method of the opposite group was repeated for each participant by switching the drugs for two more consecutive cycles. The amount of bleeding and the duration of menstruation were measured during these 5 cycles using a Higham device. Considering that the maximum effect duration of cumin is 24 hours and that of mefenamic acid capsules is 6 to 8 hours, its use on the 7th day of menstruation will not affect subsequent cycles. The mean menstrual bleeding score before treatment was 154.26±60.08, which decreased to 106.68±45.38 in the mefenamic acid group and 105.8±40.56 in the cumin group after the intervention, indicating a significant reduction. This study showed that cumin capsules can effectively reduce menstrual bleeding similarly to mefenamic acid [7].
Frankincense and Ginger
A randomized clinical trial studied the effects of ginger and frankincense on heavy menstrual bleeding. In this study, 102 patients were divided into three groups. All patients received 200mg of ibuprofen, along with 300mg of frankincense, 300mg of ginger, and a placebo that resembled the other two drugs. Patients took the medications three times a day for 7 days during their menstrual cycle, starting on the first day of menstruation and continuing for two cycles. The duration of menstrual bleeding was reduced in both the frankincense and ginger groups, but there was no significant difference in the placebo group. The amount of menstrual bleeding decreased in all groups, but there was no statistically significant difference between the groups. Quality of life also improved in both the ginger and frankincense groups, while no change was observed in the placebo group. According to the results of this study, frankincense and ginger appear to be effective complementary treatments for heavy menstrual bleeding [16].
Cinnamon
A randomized, double-blind, controlled clinical trial was conducted on 76 female students. Thirty-eight subjects received a placebo in the form of starch capsules three times a day, while 38 subjects received capsules containing 420mg of cinnamon three times a day. Pain and nausea were assessed using a visual analogue scale, and bleeding was measured using pads. Parameters were assessed during the first 72 hours of the cycle. The average amount of bleeding in the cinnamon group was significantly reduced compared to the placebo group. The level of pain in the cinnamon group was also lower than in the placebo group. Additionally, the incidence of nausea and vomiting in the cinnamon group was significantly reduced compared to the placebo group. Therefore, cinnamon was able to significantly reduce pain, nausea, and vomiting, as well as the amount of menstrual bleeding, without side effects [17].
Plantain
In a 2019 randomized, double-blind, placebo-controlled clinical trial conducted in Mashhad, 68 women aged 36 to 45 years who had heavy menstrual bleeding participated. The intervention group received placebo capsules and plantain syrup, while the control group received mefenamic acid capsules and placebo syrup during the first 5 days of the menstrual cycle for three consecutive cycles. Patients were asked about bleeding one month before the intervention, and hemoglobin levels were measured at the beginning and end of the study. The amount and duration of menstruation decreased in both groups. There was no statistically significant difference between the two groups in the severity of bleeding; however, the duration of bleeding was significantly reduced in the mefenamic acid group compared to the plantain group. Although there was a statistically significant difference in hemoglobin levels in the mefenamic acid group before and after the intervention, there was no statistically significant difference in hemoglobin levels between the two groups after the intervention. Therefore, plantain syrup can be used as a complementary treatment for heavy menstrual bleeding [13].
Chamomile
A double-blind clinical trial was conducted in 2020 involving 118 students at Guilan University of Medical Sciences. The participants were divided into two groups of 59. The intervention group took 250mg chamomile capsules three times a day, while the placebo group took a placebo three times a day, starting 7 days before the onset of menstrual bleeding. A Higham chart was used to assess the amount of blood loss during menstruation. Data were analyzed using SPSS version 20. The amount of bleeding was reduced in the chamomile group. Although statistical tests did not show a statistically significant difference in the duration and interval between two bleedings, chamomile can reduce the amount of bleeding during menstruation and can be used as a treatment method [13].
Another randomized, triple-blind clinical study was conducted in 2011 involving 90 participants in Kashan. The participants were randomly assigned to two groups: mefenamic acid and chamomile. Forty-five individuals were given mefenamic acid capsules every 8 hours, while the other 45 received 250mg chamomile capsules every 8 hours during two consecutive menstrual cycles. A Higham chart was used to determine bleeding. Data analysis was performed using SPSS version 16 software, along with the Chi-square test, Fisher’s t-test, and paired t-test. The amount of bleeding in the two treatment groups showed a statistically significant decrease compared to before treatment. In the comparison between the two drugs, the difference was not statistically significant; however, the reduction in bleeding due to chamomile and mefenamic acid in the second cycle was not different from that in the first cycle. Taking chamomile capsules can reduce menstrual bleeding and can be recommended for the treatment of heavy menstrual bleeding [18].
Golnar
A randomized, double-blind clinical trial was conducted in Qom in 2017 involving 100 participants. The participants were divided into two groups of 50. The intervention group received 500mg Golnar capsules during the first 7 days of the menstrual cycle for three consecutive cycles, while the placebo group received placebo capsules in the same manner. Bleeding duration and volume were assessed using the Higham chart, quality of life was assessed using the McGill Quality of Life Questionnaire, and hemoglobin levels were measured for 3 months. At the end of the study, 82 participants (43 in the Golnar group and 39 in the placebo group) were evaluated over the 3 months. In the Golnar group, bleeding rates were reduced, and quality of life improved, while the changes in the placebo group were not significant. Hemoglobin levels increased in the Golnar group and decreased in the placebo group. Golnar is effective for individuals who experience heavy bleeding, and it is suggested that a study with a larger sample size be conducted to investigate potential side effects [11].
Nigella
A double-blind clinical trial was conducted in 2014 involving 70 individuals at Mashhad University of Medical Sciences. The subjects were randomly assigned to the mefenamic acid and black seed groups. The study was conducted in two stages. First, all participants were screened for bleeding over two cycles. Then, each participant was randomly assigned either mefenamic acid capsules or black seed capsules for two consecutive cycles. The first group received 3 grams of black seed capsules orally daily (two 500mg capsules every 8 hours), while the second group received 250mg of mefenamic acid every 8 hours for the first 3 days of menstruation. The Hegam chart was used to assess the amount of bleeding. Data were analyzed using SPSS version 16, along with the independent t-test and the Friedman test. The mean bleeding rate in the black seed group before the intervention was 85.20±37.85, which increased to 85.62 ± 34.20 in the first treatment cycle and to 83.77±31.81 in the second treatment cycle. In the mefenamic acid group, the mean bleeding rate before the intervention was 83.77±38.31, which decreased to 78.05±32.66 in the first treatment cycle and to 76.75±29.71 in the second treatment cycle. There was no statistically significant difference between the two groups in terms of bleeding rates in the first and second cycles of treatment. Black seed can increase menstrual bleeding, but this increase was not statistically significant compared to mefenamic acid [10].
Teucrium polium
In a triple-blind clinical trial conducted in 2015 involving 70 students with primary dysmenorrhea, the effect of Teucrium polium on the duration of menstrual bleeding was investigated. The students were randomly divided into two groups of 35, with one group receiving Teucrium polium capsules and the other receiving placebo capsules. The first group was prescribed capsules containing 200mg of Teucrium polium extract four times a day during the first three days of menstruation, while the placebo group was prescribed 200mg starch-containing capsules in the same manner. The McGill Pain Questionnaire (MPQ) was used to collect data, and a questionnaire was used to assess the duration of menstrual bleeding. Data were analyzed using SPSS version 20 software, employing independent t-tests, the Mann-Whitney U test, and repeated measures ANOVA. The mean duration of menstrual bleeding before drug administration was 6.3(1.1) days in the Teucrium polium group and 6.5(2.6) days in the placebo group, with no significant difference between the two groups. The duration of menstrual bleeding in the Teucrium polium treatment group was significantly reduced compared to before treatment; however, there was no significant difference in the placebo group. Teucrium polium was more effective than a placebo in reducing menstrual bleeding. The use of Teucrium polium is recommended for the treatment of heavy menstrual bleeding and the prevention of subsequent iron deficiency anemia in women [20].
Discussion
This study aimed to systematically review clinical trials of herbal products on the severity of menstrual bleeding. Herbal remedies are part of traditional medicine. In recent years, there has been a trend toward using herbal supplements in the treatment of diseases worldwide. It is generally believed that herbal medicines are effective and have fewer side effects than chemical drugs. Many types of plants are used for female disorders, such as irregular menstrual cycles and heavy menstrual bleeding [1, 20]. Some studies have shown that certain herbal remedies are effective in reducing menstrual bleeding [13]. Calamus, black seed, marigold, chamomile, ginger, cumin, plantain, cinnamon, frankincense, fennel, yarrow, and flaxseed have been studied, and all, except for black seed, have been effective in treating heavy menstrual bleeding. Among the herbs studied, ginger, fennel, and chamomile were examined in two studies, where chamomile showed little effect on reducing menstrual bleeding, and ginger was effective in reducing bleeding in one study but not in another. In a study conducted on black seed, it was found that black seed increased menstrual bleeding, and the number of studies on other herbs was limited. Therefore, a precise conclusion and interpretation of the results of the studies cannot be drawn.
One of the plants studied is flaxseed. In a study, flaxseed powder was used. Flaxseed is the richest source of lignans, which are one of the main classes of phytoestrogens. This plant contains the essential fatty acid α-linolenic acid, which is a biological precursor to omega-3, and it also contains fiber. Lignans function as both estrogen agonists and antagonists and possess antioxidant properties. Flaxseed and lignans may have potent antiestrogenic effects on estrogen receptors. Phytoestrogens derived from flaxseed protect female reproductive tissues (such as the breast and uterus) from excessive estrogen stimulation [3].
Another plant studied in this research was yarrow. Yarrow contains inulin, phytosterols, acyl-leic acid, alkaloids, flavonoids, sesquiterpenes, oxalic acid, choline, resin, polyphenolic compounds, lactones, and tannins. This plant has antiseptic, antispasmodic, analgesic, anti-inflammatory, antioxidant, anticancer, diuretic, and estrogenic activities. Yarrow is used as an astringent for menstrual disorders, as a blood-thinning agent, as a blood-clotting agent, and as a treatment for bleeding. It has also been historically used to stop internal bleeding [4]. Yarrow contains substances, such as flavonoids, sesquiterpenes, and tannins that act as uterine smooth muscle contractants and have anti-inflammatory and antioxidant effects, which are effective in reducing severe menstrual bleeding [21].
Another plant studied in this research was Foeniculum vulgare. The parts used were the roots, leaves, and fruit, which have anti-inflammatory and antispasmodic effects. Fennel is rich in phytoestrogens, including lignans and isoflavones. The plant exhibits analgesic and antispasmodic effects on spasms caused by oxytocin and prostaglandins, and it facilitates the release of menstrual blood in a shorter period of time [6, 22].
Another plant examined was ginger. Ginger is a plant used for many disorders, such as dysmenorrhea, nausea caused by pregnancy, and skin inflammation. The anti-inflammatory effects of ginger are attributed to the modulation of prostaglandin synthesis and increased uterine smooth muscle activity. Ginger contains fat, carbohydrates, protein, fiber, water, volatile oil, monoterpenoids, sesquiterpenoids, camphene, and borneol [5]. The effect of ginger on reducing menstrual bleeding may be due to an increase in the levels of endometrial prostaglandins, such as prostaglandin F2α, prostaglandin E, and prostacyclin, which can reduce bleeding by contracting the uterine muscles. A few other studies have shown that platelet aggregation during menstrual bleeding increases with ginger consumption [2, 16].
Another studied plant was cumin. It is effective in muscle contractions and contains compounds such as carotenoids, myrcene, limonene, alpha-pinene, and beta-pinene. Studies have shown that alpha- and beta-pinene have anti-inflammatory properties, while carotenoids and limonene counteract the effects of prostaglandins. In traditional medicine, its mixture with olive oil, when applied vaginally, prevents heavy menstrual bleeding. Cumin appears to have a dual role in regulating menstruation, being effective in both treating amenorrhea and reducing menstrual bleeding [7].
Another herb studied was frankincense. In this study, frankincense and ginger were compared, and both were found to reduce menstrual bleeding. Frankincense contains boswellic acid and other five-ring triterpenes, which have a chemical structure similar to steroids. This plant is used in various countries as an anti-inflammatory, analgesic, and anti-arthritic herbal medicine, for the treatment of allergies, bronchitis, tumors, wounds, fever, diarrhea, vomiting, memory enhancement, and other conditions. Frankincense is also recommended for the treatment of eye diseases and the prevention of intestinal bleeding. However, the mechanism by which frankincense reduces bleeding has not been mentioned in studies [23].
Cinnamon was another herb studied. Cinnamon was able to significantly reduce pain, nausea, vomiting, and menstrual bleeding without any side effects. Cinnamon is an herb that has anti-inflammatory and antimicrobial properties. It contains coumarin, cinnamyl acetate, hydroxycinnamaldehyde, cinnamaldehyde, and N-acetyl-L-cysteine. These compounds belong to the benzopyrone group and are found in cinnamon, green tea, and peppermint. Cinnamon is used to treat depression, rheumatism, and muscle pain [23, 24]. According to reviews conducted in various studies, the mechanism of action of cinnamon is not mentioned.
Plantain is another plant that was studied in this research. It is used to treat conditions such as colds, wounds, fever, bleeding, and inflammation. Plantain is one of the best medicines used both orally and vaginally to reduce menstrual bleeding. The medicinal properties of this plant include antifungal, analgesic, antihemorrhagic, anti-inflammatory, phytoestrogenic, androgenic, and anemic effects. It was also able to effectively reduce menstrual bleeding [13].
Chamomile was investigated in this study. Research has shown that this plant possesses hemostatic, antiseptic, and sedative properties. Chamomile also has anti-inflammatory activity, which is attributed to compounds such as matricin (a plant alkaloid), bisabolol (a plant alkaloid), and their oxides. Chamomile contains chamazulene, which has anti-inflammatory and antioxidant effects, as well as apigenin (anti-inflammatory, sedative, and antineoplastic), flavonoids (anti-inflammatory and anti-anxiety), alpha-bisabolol (anti-inflammatory and digestive effects), alpha-heteroside, beta-heteroside, and methoxycoumarin. Additionally, chamomile has a strong antispasmodic effect. Glycine has also been found in chamomile, which can relieve uterine spasms and relax the uterus [19, 18].
Another studied plant was Golnar. Golnar is composed of six plant components, including pomegranate flowers, Persian Golnar from the family Hanaeaceae (the main component), acacia or gum arabic, clay (a compound of iron oxide), rose, tragacanth, and cinnamon oil. Golnar has an inhibitory effect on prostaglandin synthesis. Memarzadeh et al. examined the effect of pomegranate on menstrual bleeding, finding that the amount of bleeding decreases, which is consistent with this study. Golnar contains cinnamon oil, which includes tannins that have astringent properties [11].
Black seed was another studied plant. The part used in black seed is its seed, the physiological effect of which is related to the volatile oil that contains the active ingredient thymoquinone. Black seed has many properties, including antibacterial, analgesic, smooth muscle relaxant, antioxidant, anti-inflammatory, antihistamine, and protective effects on the kidney, liver, and cardiovascular tissues, as well as promoting bile and uric acid excretion and lowering sugar, fat, and blood pressure. The relaxing and antispasmodic effects of black seed have been proven in studies [10].
Teucrium polium was the last plant examined. The medicinal use of Teucrium polium dates back to the time of Hippocrates and Galen. It has a tonic and anticonvulsant effect, and its use is beneficial for treating diseases of the genitourinary system and delaying or preventing pregnancy. Studies have investigated the anti-contractile effect of Teucrium polium on the uterus. Teucrium polium, by possessing adrenergic agonist properties and increasing cAMP, causes uterine relaxation. Research conducted on Teucrium polium has shown that the plant contains tannins, triterpenoids, saponins, sterols, flavonoids, glycosides, alpha and beta pinene, and leucoanthocyanins [8, 20].
Although the results showed that these herbs have positive effects in treating heavy menstrual bleeding, the number of studies on each product is limited, making it difficult to reach a scientific and accurate decision. Therefore, better-designed studies are needed to investigate the effects of these herbs and compare their different dosage forms and dosages. Also, the mechanism of action of each of these herbs has been obtained in laboratory studies and requires further investigation in a clinical setting. Therefore, the mechanism of action of these herbs on the treatment of heavy menstrual bleeding may have differences that require further investigation and study.
These plants can affect the severity of menstrual bleeding, and although studies showed that each of these plants has different active ingredients and affects the process of reducing menstrual bleeding through different mechanisms, these plants also have common properties, such as anti-inflammatory, antibacterial, and antioxidant properties.
Conclusion
The studied plants are effective in treating heavy menstrual bleeding.
Acknowledgments: The authors would like to sincerely thank their colleagues who helped them with their advice and knowledge in writing the paper.
Ethical Permissions: Nothing declared by the authors.
Conflicts of Interests: The authors have no conflicts of interest to declare.
Authors' Contribution: Goudarzi F (First author), Introduction author/Methodologist/Main researcher/Discussion author (50%); Hekmatzadeh SF. (Second author), Introduction author/Methodologist/Assistant researcher/Statistical analyst/ Discussion author (50%);
Funding/Support: This study was supported by the Yasuj University of Medical Sciences.
Keywords:
Menstruation [MeSH], Menorrhagia [MeSH], Systematic Review [MeSH], Plants [MeSH], Plants, Medicinal [MeSH]
References
1. Javan R, Yousefi M, Nazari SM, Amiri P, Mosavi-Jarrahi A, Modiramani P, et al. Herbal medicines in idiopathic heavy menstrual bleeding: A systematic review. Phytother Res. 2016;30(10):1584-91. [Link] [DOI:10.1002/ptr.5675]
2. Kashefi F, Khajehei M, Alavinia M, Golmakani E, Asili J. Effect of ginger (zingiber officinale) on heavy menstrual bleeding: A placebo-controlled, randomized clinical trial. Phytother Res. 2015;29(1):114-9. [Link] [DOI:10.1002/ptr.5235]
3. Mirghafurvand M, Mohammadalizadeh S, Javadzadeh Y, Ahmadpour P. Comparison of the effect of Vitagenus and flaxseed on the amount of menstrual bleeding: A randomized controlled clinical trial. J Adv Med Biomed Res. 2015;23(100):1-12. [Persian] [Link]
4. Ebrahimi Varzaneh F, Nahidi F, Mojab F, Pourhoseingholi MA. Effect of Achillea millefolium on the intensity and duration of menstrual bleeding of women with menorrhagia. Iran J Obstet Gynecol Infertil. 2020;23(2):67-77. [Persian] [Link]
5. Shirooye P, Hamzeloo-Moghadam M, Hashem-Dabaghian F, Mokaberinejad R. Comparison of local effects of ginger oil with oral ginger on associated symptoms of primary dysmenorrhea: Randomized clinical trial. Iran J Obstet Gynecol Infertil. 2017;20(8):61-9. [Persian] [Link]
6. Bokaie M, Enjezab B. The effects of oral fennel extract on the intensity of menstrual bleeding in relieving dysmenorrheal: A randomized clinical trial. J Community Health. 2014;8(1):55-62. [Persian] [Link]
7. Rajabi Naeeni M, Modarres M, Amin G, Bahrani N. A comparative study of the effects of cumin and mefenamic acid capsules on menstrual bleeding in IUD users: A randomized triple blind clinical trial. J Med Plants. 2015;14(54):159-68. [Persian] [Link]
8. Reza Pourahmdi M, Mehrabi Y, Keshavarz Z, Abadian K, Shirmohamadi Hesari Z. The effect of Teucrium polium capsules on the trend of primary dysmenorrhea using pair copula Bayesian network. Iran J Obstet Gynecol Infertil. 2019;22(3):41-8. [Persian] [Link]
9. Sourteji A, Kariman N, Mojab F, Alavi Majd H. Comparison of the effect of mefenamic acid and the hydroalcoholic extract of Urtica dioica on the volume of heavy menstrual bleeding in students at Azad University of Babol (2011-2012). J Arak Univ Med Sci. 2013;16(4):27-36. [Persian] [Link]
10. Jafarnejad F, Mohanazadeh Falahieh F, Rakhshandeh H, Shakeri MT. Comparison of the effect of nigella sativa and mefenamic acid on menstrual hemorrhage in the students with primary dysmenoreha. Iran J Obstet Gynecol Infertil. 2016;18(185):10-5. [Persian] [Link]
11. Yousefi F, Kashanian M, Nazem I, Bioos S, Sadeghpour O, Alias J, et al. Comparison between Golnar product and placebo in heavy menstrual bleeding: A double-blind randomized clinical trial. Avicenna J Phytomed. 2020;10(5):523-32. [Link]
12. Rahi P, Mirghafourvand M, Mohammad-Alizadeh-Charandabi S, Javadzadeh Y, Seidi S. Comparison of the effect of mefenamic acid and quince on the level of menstrual bleeding and hemoglobin: A randomized controlled clinical trial. Eur J Integr Med. 2016;8(1):67-72. [Link] [DOI:10.1016/j.eujim.2015.11.022]
13. Khodabakhsh M, Mahmoudinia M, Bazaz MM, Hamedi SS, Hoseini SS, Feyzabadi Z, et al. The effect of plantain syrup on heavy menstrual bleeding: A randomized triple blind clinical trial. Phytother Res. 2020;34(1):118-25. [Link] [DOI:10.1002/ptr.6502]
14. Hopewell S, Boutron I, Moher D. CONSORT and its extensions for reporting clinical trials. In: Principles and practice of clinical trials. Cham: Springer; 2020. p. 1-15. [Link] [DOI:10.1007/978-3-319-52677-5_188-1]
15. Akhavan Amjadi M, Zahrani S, Mojab F, Alavi Majd H. Efficacy of foeniculum vulgare mill extract on menstrual bleeding over the students of Shahid Beheshti University in Tehran 2005. J Med Plants. 2010;9(34):117-23. [Persian] [Link]
16. Eshaghian R, Mazaheri M, Ghanadian M, Rouholamin S, Feizi A, Babaeian M. The effect of frankincense (Boswellia serrata, oleoresin) and ginger (Zingiber officinale, rhizoma) on heavy menstrual bleeding: A randomized, placebo-controlled, clinical trial. Complement Ther Med. 2019;42:42-7. [Link] [DOI:10.1016/j.ctim.2018.09.022]
17. Jaafarpour M, Hatefi M, Najafi F, Khajavikhan J, Khani A. The effect of cinnamon on menstrual bleeding and systemic symptoms with primary dysmenorrhea. Iran Red Crescent Med J. 2015;17(4):e27032. [Link] [DOI:10.5812/ircmj.17(4)2015.27032]
18. Mollabashi EN, Ziaie T, Bekhradi R, Khalesi ZB. Do Chamomile effect on duration, amount of bleeding, and interval of menstrual cycles?. J Pharmacopuncture. 2020;23(1):25-9. [Link] [DOI:10.3831/KPI.2020.23.004]
19. Karimian Z, Sadat Z, Bahrami N, Kafaie M. Comparison of chamomile and mefenamic acid capsules in hemorrhage of menstruation. Iran J Obstet Gynecol Infertil. 2015;18(157):11-7. [Persian] [Link]
20. Shirmohamai Hesari Z, Zayeri F, Abadian K, Keshavarz Z, Akbari Nozari M. The effect of Teucrium polium capsule on pain duration of primary dysmenorrhea. Iran J Obstet Gynecol Infertil. 2018;21(8):66-74. [Persian] [Link]
21. Bagheri A, Amin G, Tavangar SM, Heidari M, Bagheri J. Safety and hemostatic effect of Achillea millefolium L. in localized bleeding. Hepatol Forum. 2024;5(1):25-7. [Link] [DOI:10.14744/hf.2022.2022.0041]
22. Motavalli R, Shahbazzadegan S. The effect of fennel on the amount and duration of menstrual bleeding: A quasi-experimental study. Iran J Obstet Gynecol Infertil. 2024;27(1):55-62. [Persian] [Link]
23. Parandin R, Sadeghipour Rodsari H, Shamili S, Ghasempour H. Effects of aqueous extract of boswellia thurifera on fertility in male rats. J Adv Med Biomed Res. 2008;16(65):23-30. [Persian] [Link]
24. Bakar A, Yao PC, Ningrum V, Liu CT, Lee SC. Beneficial biological activities of Cinnamomum osmophloeum and its potential use in the alleviation of oral mucositis: A systematic review. Biomedicines. 2020;8(1):3. [Link] [DOI:10.3390/biomedicines8010003]










